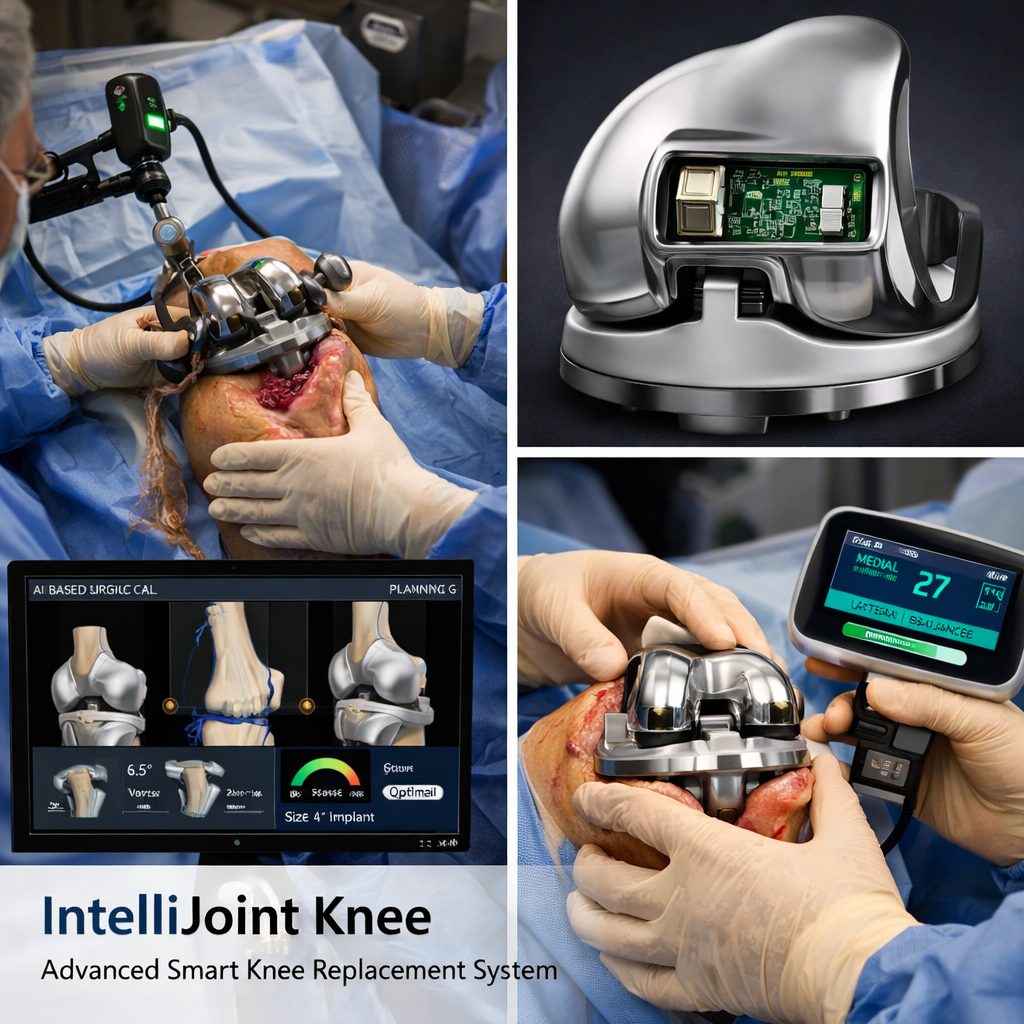
Total Knee Replacement (TKR) has undergone a remarkable evolution from conventional, mechanically aligned procedures to highly advanced, technology-driven interventions aimed at improving precision, reproducibility, and patient-specific outcomes. Traditional TKR techniques relied on intramedullary and extramedullary guides, with surgical success largely dependent on the surgeon’s experience and intraoperative judgment. Although these methods have demonstrated excellent long-term survivorship, limitations such as variability in alignment, subjective soft tissue balancing, and suboptimal functional outcomes in a subset of patients have driven the search for more refined approaches. The introduction of robotic-assisted TKR represented a significant milestone, enabling improved accuracy of bone resections, better implant positioning, and enhanced reproducibility. However, robotic systems primarily address the execution of surgery and remain dependent on preoperative planning and surgeon-defined parameters, with limited capacity for real-time intraoperative decision-making.
The next phase in this evolution is the emergence of intelligent knee systems, particularly IntelliJoint knee technologies, which represent a paradigm shift toward data-driven, personalized arthroplasty. IntelliJoint knee integrates advanced intraoperative sensors, artificial intelligence, and real-time analytics to provide objective, quantifiable data on joint biomechanics during surgery. These systems allow precise assessment of medial and lateral compartment loads, enabling accurate and reproducible ligament balancing, which has traditionally been subjective. Furthermore, IntelliJoint technology facilitates dynamic evaluation of knee kinematics throughout the range of motion, guiding surgeons in achieving optimal alignment tailored to the individual patient rather than adhering strictly to conventional mechanical targets.
A key innovation of IntelliJoint knee systems is the incorporation of smart implant technology, where embedded micro-sensors can monitor joint loading patterns, activity levels, and functional performance postoperatively. This continuous feedback loop extends beyond the operating room, allowing for remote monitoring, early detection of complications, and optimization of rehabilitation protocols. Additionally, AI-based preoperative planning tools can analyze patient-specific anatomical and functional data to predict optimal implant positioning and expected outcomes, thereby enhancing surgical planning and intraoperative adaptability.
By shifting the focus from purely mechanical alignment to functional and personalized alignment strategies, IntelliJoint knee technology addresses one of the primary causes of dissatisfaction following TKR—namely, the inability to replicate natural knee kinematics. It transforms TKR from a procedure based on generalized principles into a highly individualized intervention guided by real-time data and predictive analytics. Although challenges such as cost, accessibility, and the need for long-term outcome validation remain, IntelliJoint knee systems represent a significant advancement toward precision medicine in orthopedics.
In conclusion, while robotic-assisted TKR has improved surgical precision, the advent of IntelliJoint knee technology marks the transition toward intelligent arthroplasty, where intraoperative decision-making is augmented by objective data and postoperative care is enhanced through continuous monitoring. This integration of sensors, artificial intelligence, and digital health platforms is poised to redefine the future of knee replacement surgery, with the potential to improve functional outcomes, increase patient satisfaction, and set new standards in personalized orthopedic care.
Dr. Raghavendra Naveen, an experienced orthopedic practitioner with a strong clinical focus on arthroplasty and rehabilitation, emphasizes that the incorporation of IntelliJoint knee technology into routine practice represents not only a technological advancement but also a fundamental shift toward patient-centric, outcome-driven care in modern orthopedics.




